Study Reveals Limitations of Traditional Blood Pressure Measurement
Understanding Blood Pressure
A recent study suggests that conventional methods of measuring blood pressure may not provide adequate information to prevent premature mortality. Blood pressure is generated when the heart beats, pushing blood through the arteries. This action creates pressure within the blood vessels, which is referred to as systolic pressure. Conversely, diastolic pressure is defined as the pressure in the arteries when the heart is resting between beats. Blood pressure readings are typically expressed as a fraction, with systolic pressure on the top and diastolic pressure on the bottom.
Both systolic and diastolic numbers are crucial in evaluating heart health. Readings exceeding 120/80 indicate that the heart is exerting excessive effort to circulate blood. A diagnosis of hypertension, or high blood pressure, is generally made when measurements exceed 140/90. Accurate blood pressure measurement is essential, as individuals with hypertension face an elevated risk of heart disease, stroke, and mortality. Globally, hypertension stands as the leading cause of premature death and disability.
Current Blood Pressure Measurement Methods
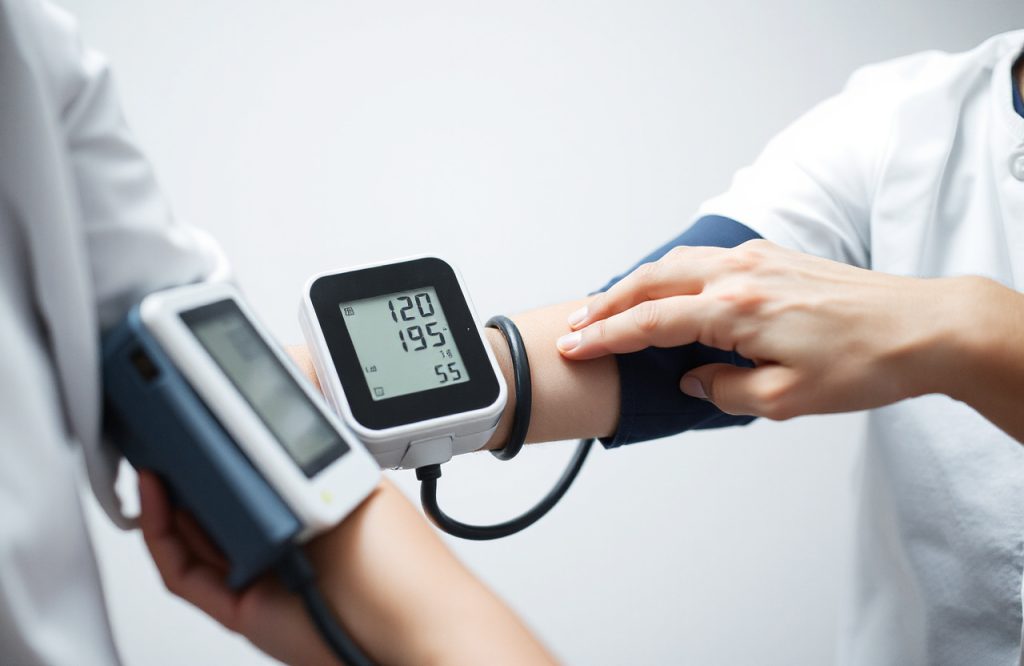
Traditionally, hypertension diagnosis involves using a blood pressure cuff placed around the upper arm during a clinic or doctor’s office visit. However, blood pressure readings taken in-office may sometimes appear normal, despite elevated overall blood pressure levels, a condition known as “masked” hypertension. Conversely, anxiety or stress associated with medical visits can cause artificially high readings, termed “white coat” hypertension. Both scenarios can lead to misdiagnosis and inappropriate treatment, increasing the risk of cardiovascular events, stroke, and death.
Exploring Advanced Measurement Techniques
Is there a more effective way to identify hypertension and reduce the risk of premature death? Ambulatory blood pressure (ABP) monitoring presents an alternative method. This technique utilizes an oscillometric device to measure blood pressure every 20 minutes during the day and every half hour at night over a 24-hour period.
A study published in the New England Journal of Medicine conducted by Spanish researchers compared in-office blood pressure monitoring to 24-hour ABP monitoring to determine which method more accurately identifies hypertension and cardiovascular mortality. The researchers analyzed data from nearly 64,000 adult Spanish patients with hypertension, recruited between 2004 and 2014. Each participant underwent both in-office blood pressure assessments and 24-hour ABP monitoring.
Key Findings on Mortality Predictions
During a median follow-up period of 4.7 years, the study revealed that 2,513 individuals died from any cause, with an additional 1,295 succumbing to cardiovascular disease. The research team concluded that ABP monitoring was significantly more effective at predicting both cardiovascular and overall mortality than traditional in-office measurements. Notably, masked hypertension was found to be the most strongly linked to mortality risks. Additionally, even white-coat hypertension showed a heightened mortality risk compared to individuals with normal blood pressure.
This study indicates that ABP monitoring offers more valuable insights than in-office measurements, suggesting it should be utilized to enhance the diagnosis and treatment of hypertension.
Reference
Banegas, J. R., Ruilope, L. M., de la Sierra, A., Vinyoles, E., Gorostidi, M., de la Cruz, J. J., … & Williams, B. (2018). Relationship between clinic and ambulatory blood-pressure measurements and mortality. New England Journal of Medicine, 378(16), 1509-1520. DOI: 10.1056/NEJMoa1712231
Related Topics of Interest
– How do smoking, diabetes, and blood pressure affect heart attacks in women?
– Developers test new blood pressure app for iPhone
– Southern diet plays a large role in the risk of high blood pressure
– Can a smartphone app help you manage your blood pressure medications?