Introduction to Complementary and Alternative Medicine
Complementary and alternative medicine (CAM) is gaining traction in healthcare settings across Western countries, often used in conjunction with or as a substitute for conventional Western medicine. The National Centre for Complementary and Integrative Health defines CAM as a broad spectrum of non-conventional health practices and products, including dietary supplements, meditation, and chiropractic manipulation.
Understanding Acupuncture
Acupuncture, a prominent form of CAM, is increasingly recognized for its effectiveness in treating various conditions, particularly acute and chronic pain.
Origins of Acupuncture
This practice has its roots in Traditional Chinese Medicine (TCM), a medical system that has been utilized for thousands of years in China. Although TCM has historical ties to Japan and Korea, its principles and practices have only recently gained popularity in Western countries over the last century. TCM encompasses not only acupuncture but also herbal remedies and Tai Chi, which emphasizes mindful movements and breathing.
Holistic Approach of TCM
Traditional Chinese Medicine is founded on a holistic philosophy that emphasizes the interconnectedness of the body. It describes a network of channels, known as meridians, that link all bodily parts. Qi, or vital energy, flows through these meridians to maintain health and wellness. According to TCM, health issues arise when blockages disrupt the normal flow of qi.
Mechanism of Acupuncture
The goal of acupuncture is to restore the flow of energy by using needles to unblock these channels at specific points where blockages may exist. While acupuncture has been applied to various symptoms and diseases, research indicates that it is particularly effective for pain relief, including conditions like lower back pain, shoulder pain, neck pain, menstrual cramps, migraines, and insomnia.
How Acupuncture Treatment Works
Acupuncture treatment typically begins with the practitioner conducting a general physical examination and gathering the patient’s medical history. The practitioner then identifies specific acupuncture points based on the patient’s symptoms.
Identification of Acupuncture Points
The identification of these points has been extensively studied, yet remains a topic of ongoing research. In TCM, acupuncture points were identified through centuries of observation regarding symptom relief when specific tender spots were stimulated. Consequently, practitioners choose points based on the nature and location of the patient’s symptoms.
Procedure of Acupuncture
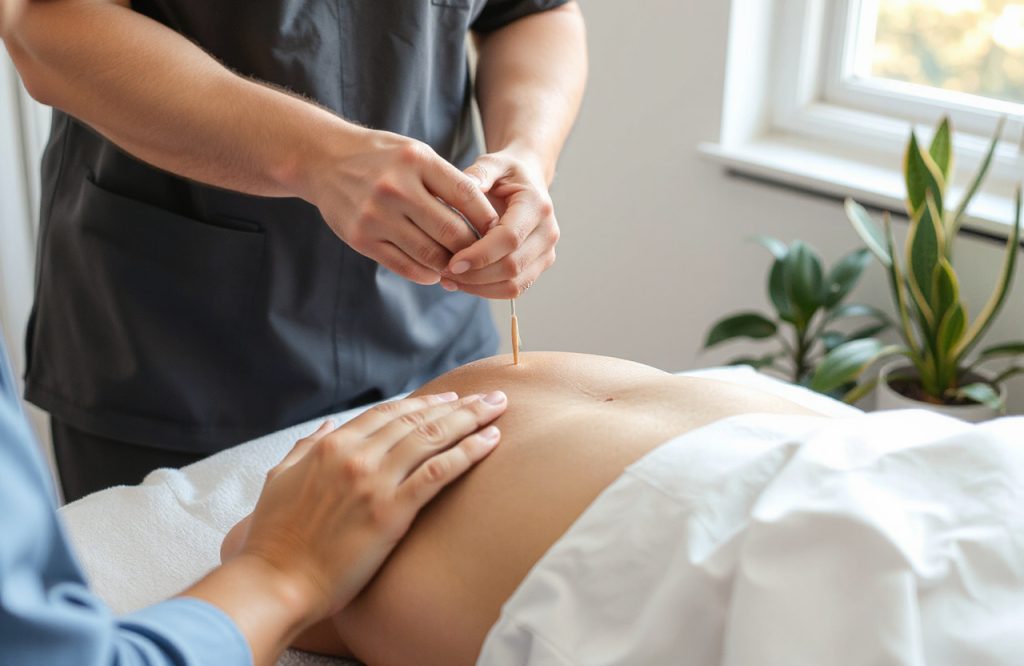
After determining the relevant acupuncture points, the practitioner inserts between five and twenty small sterile needles into the body. Patients often report a sensation of numbness upon insertion, which is considered a sign of the treatment’s effectiveness. The needles typically remain in place for 10 to 30 minutes. In addition to needles, acupuncture points can also be stimulated using mild electromagnetic stimulation or heat.
Importance of Treatment Environment
The environment where acupuncture is performed plays a critical role in treatment effectiveness. Ideally, it should be a quiet and calming space. While the exact mechanisms through which acupuncture exerts its effects are not fully understood, research suggests that it may help block or delay pain signals being transmitted to the brain, thereby reducing pain perception. Additionally, needle insertion may trigger the release of neurotransmitters, which are natural pain-relieving chemicals produced by the body.
Effectiveness of Acupuncture
The number of rigorous clinical trials assessing the efficacy of acupuncture has grown, providing substantial evidence of its effectiveness, particularly for pain relief.
Clinical Trial Findings
Research indicates that acupuncture is generally more effective for pain relief compared to no treatment or sham acupuncture, where needles are placed at non-acupuncture points. Some studies suggest that the difference in pain relief between real and sham acupuncture is not statistically significant. Nonetheless, most studies agree that both types of acupuncture treatments outperform no treatment or standard care. Furthermore, combining acupuncture with conventional medicine may enhance pain relief compared to using medication alone.
Safety of Acupuncture
Acupuncture is generally regarded as a safe treatment for most individuals, with certain exceptions such as ongoing infections or neutropenia—conditions that heighten infection risks. It is frequently utilized by vulnerable populations, including pregnant women.
Potential Complications
While both minor and serious complications can occur, they are rarely experienced according to safety studies. Potential complications include infection, bleeding, and nerve or tissue damage. Proper sterilization of needles and treatment by trained practitioners significantly reduces these risks.
Training and Certification of Practitioners
Acupuncture practitioner training varies by state. Generally, practitioners undergo one of two qualification processes: clinical or non-clinical acupuncture certification. Clinical certification, awarded by the American Board of Medical Acupuncture, requires a standardized exam and completion of 200 to 300 hours of acupuncture training following a four-year medical program. Non-clinical acupuncturists receive certification from the National Certification Commission for Acupuncture and Oriental Medicine after completing a three-year Master’s program in acupuncture and passing a certification exam.
Conclusion
While acupuncture appears to be an effective and safe option for various symptoms and conditions, the National Centre for Complementary and Integrative Health advises consulting a healthcare provider before considering acupuncture as a complementary treatment to conventional care.
References
Chan, M., Wu, X. Y., Wu, J., Wong, S., & Chung, V. (2017). Safety of acupuncture: Overview of systematic reviews. Scientific Reports, 7(1), 3369. https://doi.org/10.1038/s41598-017-03272-0
Kawakita, K., & Okada, K. (2014). Acupuncture therapy: mechanism of action, efficacy, and safety: A potential intervention for psychogenic disorders?. BioPsychoSocial Medicine, 8(1), 4. https://doi.org/10.1186/1751-0759-8-4
Lim, T. K., Ma, Y., Berger, F., & Litscher, G. (2018). Acupuncture and Neural Mechanism in the Management of Low Back Pain-An Update. Medicines, 5(3), 63. https://doi.org/10.3390/medicines5030063
National Centre for Complementary and Integrative Health. (2018). Complementary, alternative, or integrative health: What’s in a name? Retrieved from https://www.nccih.nih.gov/health/complementary-alternative-or-integrative-health-whats-in-a-name
National Certification Commission for Acupuncture and Oriental Medicine. (n.d.). The NCCAOM certification in acupuncture. Retrieved from https://www.nccaom.org/wp-content/uploads/pdf/NCCAOM%20Acupuncture%20Certification%20Fact%20Sheet060318.pdf
Van Hal, M., DyDyk, A. M., & Green, M. S. (2020). Acupuncture. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK532287/#_NBK532287_pubdet
Vickers, A. J., & Linde, K. (2014). Acupuncture for chronic pain. Journal of the American Medical Association, 311(9), 955–956. https://doi.org/10.1001/jama.2013.285478