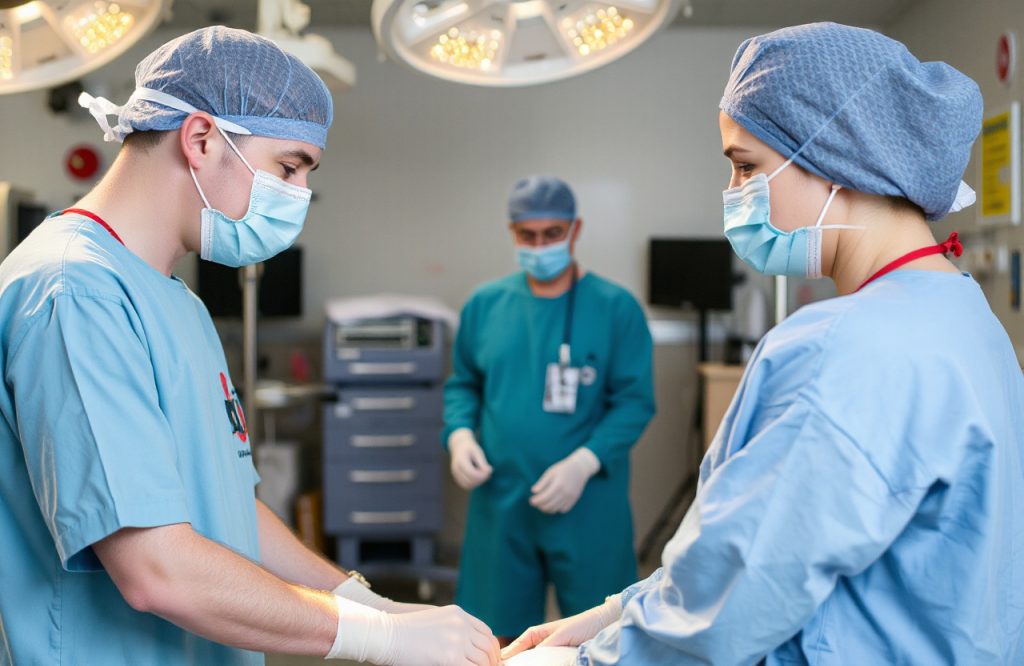
Study Reveals COVID-19 Risk Among Hospital Staff
Background on Occupational Exposure
A recent study from a prominent UK medical center highlights that intensive care staff faced the lowest risk of contracting COVID-19 during the peak of the pandemic. Since the onset of the SARS-CoV-2 pandemic, the occupational exposure risk for healthcare workers has raised significant concerns. Research indicates that healthcare professionals experience higher infection rates compared to the general population, with rates of up to 14% in symptomatic and 7.1% in asymptomatic hospital staff.
Study Overview
The University Hospitals Birmingham NHS Foundation Trust (UHBFT), one of the largest hospital trusts in the UK, conducted a cross-sectional study involving 554 staff members. The primary goal was to assess the point prevalence of infection and the seroprevalence of SARS-CoV-2 antibodies among healthcare workers. The study also aimed to explore the relationship between prior COVID-19 symptoms and the departments in which participants worked. Insights gained from this research are vital for understanding herd immunity, vaccine development, and strategies to protect healthcare workforces.
Methods of Participant Recruitment
The study engaged 545 asymptomatic healthcare workers who were invited to participate via UHBFT’s social media channels. Participants were excluded if they exhibited current symptoms indicative of COVID-19. Each participant underwent a nasopharyngeal swab and a venous blood sample to test for SARS-CoV-2 RNA and anti-SARS-CoV-2 spike glycoprotein antibodies, respectively.
Key Findings
Published in the journal Thorax, the results revealed that intensive care staff had the lowest incidence of COVID-19 infection during the pandemic’s height. Conversely, cleaners, clinicians in acute and general medicine, and individuals from Black, Asian, and Minority Ethnic (BAME) backgrounds were identified as the most vulnerable to infection. Among the asymptomatic healthcare staff, nearly 2.5% tested positive for SARS-CoV-2, with 38% later developing symptoms. Furthermore, 26% reported having previously experienced symptoms consistent with COVID-19, and those with prior symptoms were significantly more likely to have antibodies compared to those without symptoms. The overall seroprevalence was noted at 24%, markedly higher than the 6% observed in the wider Midlands area at that time.
Impact of Personal Protective Equipment
Researchers suggest that the lower infection rates among intensive care clinicians can be attributed to the use of enhanced personal protective equipment (PPE), including mandatory filtered facepiece (class 3) respirators. In contrast, other clinical areas primarily utilized fluid-resistant surgical masks. The effectiveness of enhanced PPE in safeguarding staff from SARS-CoV-2 infection warrants further investigation, along with the necessity for adequate training, space, and supervision for proper PPE utilization.
Implications for Future Healthcare Planning
The data gathered from this study offers valuable insights for future strategies aimed at protecting healthcare workers during potential surges in COVID-19 cases or subsequent pandemics. Additionally, the insights could inform responses to seasonal influenza impacts on healthcare services and personnel each winter.
Source
Written by Helen Massy, BSc.
References:
EurekAlert!. 2020. Hospital COVID-19 Risk Lowest Among Intensive Care Staff. [online] Available at: [Accessed 16 September 2020].
Shields, A., et al. 2020. SARS-CoV-2 seroprevalence and asymptomatic viral carriage in healthcare workers: a cross-sectional study. Thorax, pp.thoraxjnl-2020-215414.
Image by cromaconceptovisual from Pixabay.